Spinal cord stimulation (SCS) involves the delivery of pulsed electric signals near the spinal cord to reduce and control pain for certain medical conditions. It was originally described by Shealy in 1967. Since its introduction, major improvements and discoveries have helped us understand how SCS works, for which conditions it is beneficial and the optimal equipment design.
Technique and Mechanism of Action
Unfortunately, the effective treatment of chronic pain cannot always be achieved with non-invasive pain treatments. SCS may be considered when other treatments such as medical management, surgical intervention, and physical therapy have not been effective in relieving pain.
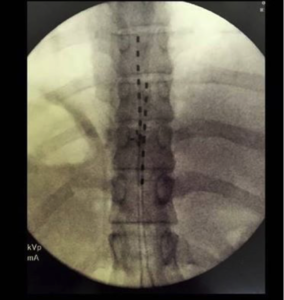
Two stages are involved in SCS. In both, a physician, guided by an x-ray, places a lead into the epidural space located within the bony spinal canal. The first stage is the trial phase which provides information to predict the success of permanent implantation.
During the trial phase, one or two leads are placed via an epidural needle in the appropriate position. This is an outpatient procedure under light sedation. Once the lead is in position, it is tested to see if the patient’s painful area is covered with a tingling sensation (paresthesia). It is important that the patient is alert during the insertion and testing of the lead so they can inform the healthcare provider if the lead is in the appropriate position.
The lead is programmed with a computer. The patient then goes home for three to five days. He or she has an external power source and remote control that allows him or her to control the amount of stimulation being received. During the trial, the patient determines if the treatment is helpful in relieving pain and improving function. At the end of the trial, the patient returns to the physician’s office to discuss the results and have the lead removed.
Together, the healthcare provider and the patient decide whether or not to advance to permanent implantation. In this stage, the lead is again placed and implanted underneath the skin with a power source the size of a pacemaker battery. Rechargeable batteries can extend the life of the battery, giving the patient up to nine years before a replacement battery must be surgically placed. The SCS recipient goes home with a remote-control and battery charger. Their activity is limited for approximately 12 weeks to allow for healing.
Medical researchers are still investigating how SCS controls pain and are considering multiple theories. One is the gate control theory, which was the originally proposed mechanism of action of SCS. This theory states that by providing a pleasant vibratory and touch sensation via the SCS system, pain signals that reach the brain are decreased. Recently, we have discovered that spinal cord stimulation modifies the chemical makeup of the spinal cord.
Some people respond better to SCS than others, which is why selecting the right individuals is so important.
Prior to SCS treatment, patients should have trialed more conservative therapies and have undergone psychological screening to make sure that underlying psychological conditions have been addressed and effectively treated. Furthermore, it is important for the patient and healthcare provider to have realistic expectations regarding treatment, with the goal being pain reduction and control rather than complete elimination.
Currently, conditions that can respond favorably to SCS treatment include:
• Post-laminectomy pain syndrome (persistent pain after neck or back surgery)
• Complex regional pain syndrome (previously known as RSD and causalgia)
• Peripheral neuropathic pain
• Peripheral vascular disease
• Ischemic heart disease
SCS has been proven to be effective for many of these conditions with lasting results in terms of pain relief, pain medication reduction, and improvement in quality-of-life indices and satisfaction scores.
For example, approximately 10 to 40 percent of people in United States that have had previous surgery for back pain continue to have significant pain. Compared to another operation for persisting back and extremity pain, SCS is often more clinically effective and more cost effective.
Although there are significant upfront costs for SCS, the treatment often reduces costs in the long run secondary to its efficacy and reduction in healthcare services used by patients with SCS. A significant advantage of a SCS system is that it is a reversible and nondestructive treatment option. It can also be effective for inoperable peripheral vascular disease (PVD).
In the United States more than eight million people are affected by PVD. In some of these individuals, SCS may improve microcirculation (i.e. blood flow), reduce pain, increase walking distance, and promote ulcer healing. However, one must remember that PVD is often a progressive disease
The Beginning of a Long-Term Relationship
Effectively treating pain by implanting an SCS system requires a responsive, long-term relationship between the person with pain and his or her healthcare provider. Occasional re-programming will be needed to optimize coverage of the painful area.
As with most treatments for chronic pain, it is important for people with SCS to involve themselves in a multidisciplinary treatment plan if they are to get the best results. In appropriately selected individuals, SCS treatment can be an important tool in a treatment plan and significantly reduce pain and associated limitations.
Over the past 30 years, Spinal Cord Stimulation (SCS) has greatly changed in the way that pain is managed. SCS involves the delivery of pulsed electric signals near the spinal cord to reduce and control pain. Spinal Cord Stimulation is a clinically effective method to manage chronic pain resulting from such conditions as post laminectomy pain syndrome (pain after previous neck or back surgery), complex regional pain syndrome, and peripheral neuropathic pain. Since its introduction, major improvements and discoveries have helped us understand how SCS works, for which condition it is beneficial, and the optimal equipment design.
One major advancement has been the development of high frequency 10 kilohertz (HF10) therapy which provides pain control without the tingling and buzzing feelings known as paresthesias. Traditional SCS therapy works on a paresthesia based platform. High Frequency-10 stimulation deliver electrical stimulation at 10 kilohertz, which modifies the nerves delivering pain signals without the tingling sensation felt with traditional stimulation. Many patient prefer paresthesia free stimulation. HF10 therapy has been shown to be very effective for chronic back and leg pain. A study by Al-Kaisy et al. showed that 88% of patients who underwent a HF-10 trial had significant reductions in pain scores and underwent permanent implantations. Another study by Kapural et al. concluded that HF10 therapy was also found to be highly clinically effective in the treatment of chronic back and leg pain and that 78.7% of patients were responders for leg and back pain (> 50% pain relief) at 12 months. Like other methods of SCS therapy, HF-10 therapy provides the opportunity for patients to undergo a trial for the system in order to assess whether HF10 is a viable option for managing your specific pain prior to undergoing the implantation stage.
References:
Al-Kaisy A, Van Buyten JP, Smet I, Palmisani S, Pang D, Smith T: Sustained effectiveness of 10 kHz high-frequency spinal cord stimulation for patients with chronic, low back pain: 24-month results of a prospective multicenter study. Pain Med 2014; 15: 347-54.
Kapural L, Yu C, Doust MW, Gliner BE, Vallejo R, Sitzman BT, Amirdelfan K, Morgan DM, Brown LL, Yearwood TL, Bundschu R, Burton AW, Yang T, Benyamin R, Burgher AH: Novel 10-kHz High-frequency Therapy (HF10 Therapy) Is Superior to Traditional Low-frequency Spinal Cord Stimulation for the Treatment of Chronic Back and Leg Pain: The-RCT Randomized Controlled Trial. Anesthesiology 2015; 123: 851-60.
Contact form
Or just call (412) 221-7640 and we’ll do everything we can to help.
Across all review platforms
Dr. David Provenzano, a leading expert throughout the nation for treating patients who suffer daily from pain, uses advanced diagnostic techniques to assess the source of the pain and develop a comprehensive and safe treatment approach that can significantly reduce your pain.